Chronic Venous Insufficiency (CVI)
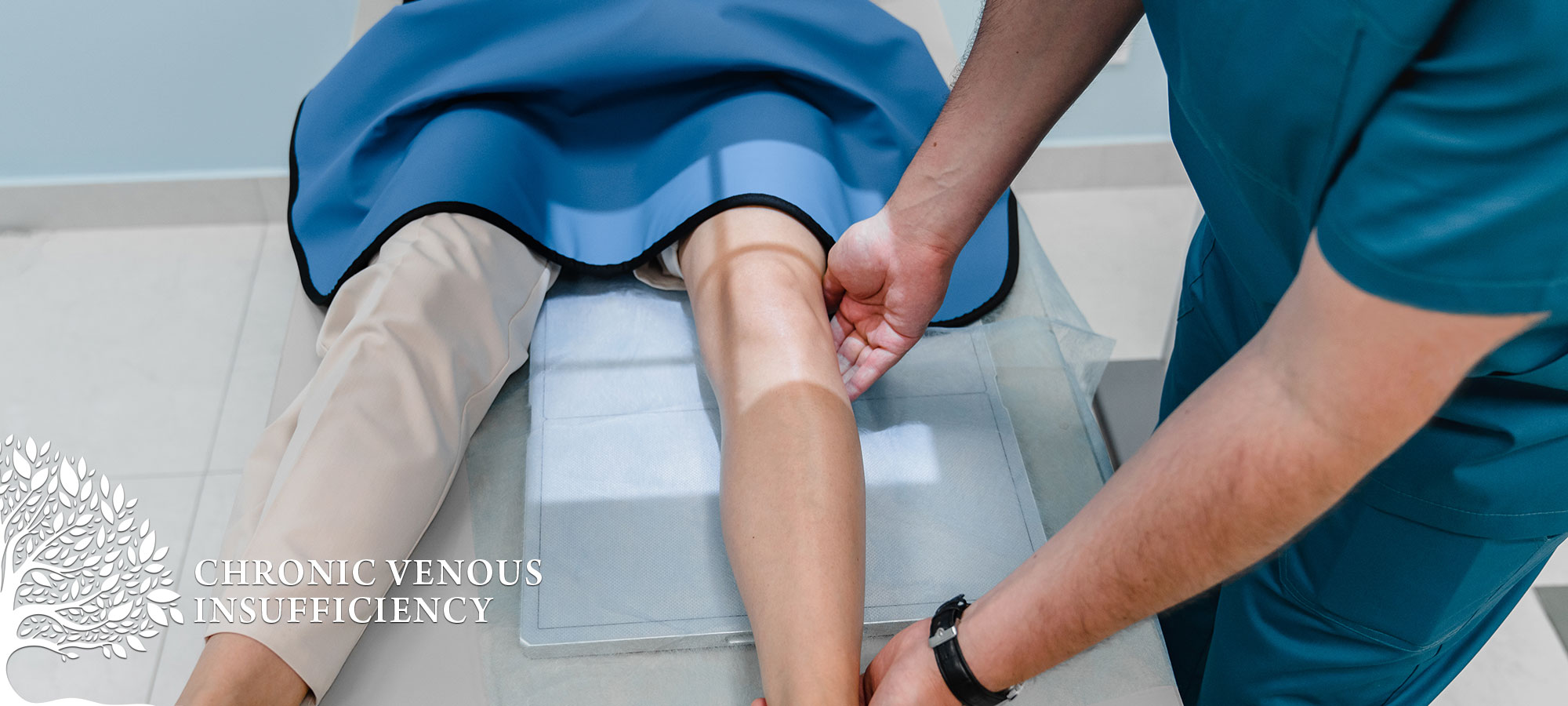
Chronic Venous Insufficiency (CVI) is a common cardiovascular condition caused by malfunctioning valves in the veins of the lower legs. Normally, blood returns to the heart through regular leg movements like walking. When the valves fail to work correctly, blood can pool in the lower legs, leading to increased pressure, discomfort, and potential complications if left untreated. Approximately 150,000 new cases of CVI are diagnosed annually in the U.S., with an estimated $500 million spent on patient care. Women over 50, especially those with a history of multiple pregnancies, are most commonly affected.
Causes of Chronic Venous Insufficiency
CVI can develop due to several contributing factors, including:
• Family history of vein issues
• Aging process
• Multiple pregnancies
• Prolonged sitting or standing jobs
• Obesity
• Vein damage or previous Deep Vein Thrombosis (DVT)
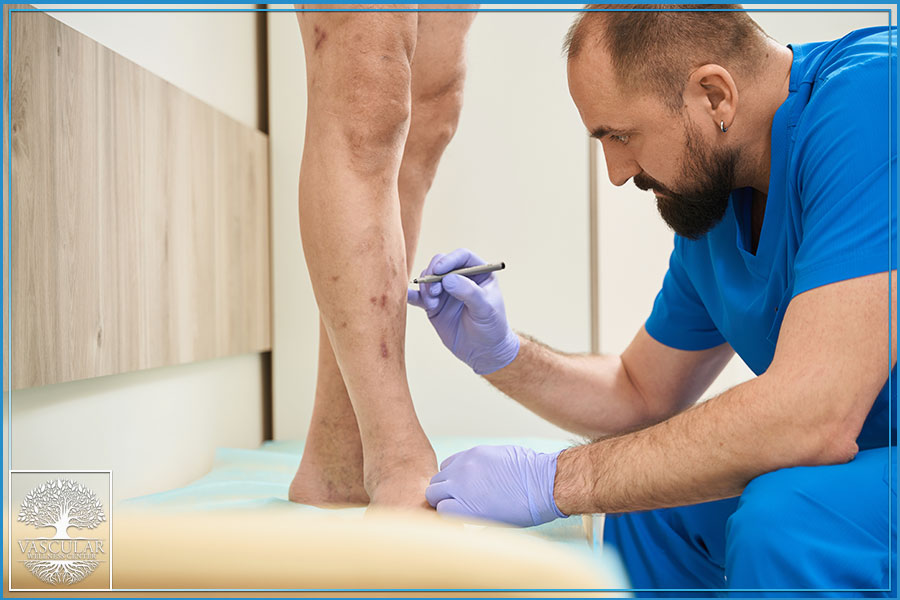
Causes of Chronic Venous Insufficiency
CVI can develop due to several contributing factors, including:
• Family history of vein issues
• Aging process
• Multiple pregnancies
• Prolonged sitting or standing jobs
• Obesity
• Vein damage or previous Deep Vein Thrombosis (DVT)
Risk Factors and Symptoms of CVI
Certain factors can increase the risk of developing CVI, such as:
• Lack of regular exercise
• Long periods of sitting or standing
• Obesity
• Aging
• Pregnancy
• Smoking
Common Symptoms Include:
• Swelling in the lower legs
• Painful varicose veins
• Leathery skin texture
• Itching, burning, or pain in the legs
• Brownish discoloration of the lower legs (hyperpigmentation)
• Non-healing wounds or ulcers on the lower extremities
Diagnosing Chronic Venous Insufficiency
CVI can be diagnosed through a venous duplex ultrasound, a non-invasive imaging test performed in an outpatient setting. This test evaluates blood flow and identifies any abnormalities in the veins, guiding the choice of treatment.
Treatment Options for CVI
Treatment depends on the severity of the condition. In mild cases, lifestyle modifications can significantly reduce symptoms and disease progression. More advanced stages may require medical procedures.
Non-Invasive Treatments:
• Lifestyle changes (diet, weight management, regular exercise)
• Compression stockings to improve blood circulation
• Elevation of the legs to reduce swelling
Advanced Medical Treatments:
• Thermal Ablation: Heat is used to close off abnormal veins.
• Chemical Ablation: Medication is injected to seal the vein.
• Venoplasty and Stenting: In severe cases, ballooning and stenting can open and stabilize blocked veins.
Preventing Chronic Venous Insufficiency
Simple lifestyle adjustments can help prevent or slow the development of CVI, such as:
• Quitting smoking
• Maintaining a healthy weight
• Adopting a balanced diet with limited fat and cholesterol
• Engaging in regular physical activity
• Avoiding prolonged sitting or standing
• Wearing supportive shoes and compression stockings

CVI Progression and Complications
If left untreated, CVI can lead to worsening symptoms such as:
• Varicose and spider veins
• Increased swelling and leg pain
• Skin discoloration and texture changes
• Open sores or ulcers, which can be difficult to treat
FAQs About CAS:
What are the symptoms of CVI?
Symptoms may include swelling, cramping, heaviness, varicose veins, skin changes, and non-healing wounds or ulcers.
How is CVI treated?
Mild cases can be managed with compression stockings and lifestyle changes, while more advanced cases may require venous procedures like thermal or chemical ablation and stenting.
Who is most affected by CVI?
CVI affects around 50% of U.S. adults, with women over 50, particularly those with multiple pregnancies, being at the highest risk.
What can I do to prevent CVI?
Preventive measures include maintaining a healthy lifestyle, avoiding smoking, regular exercise, and wearing supportive shoes and compression gear.
