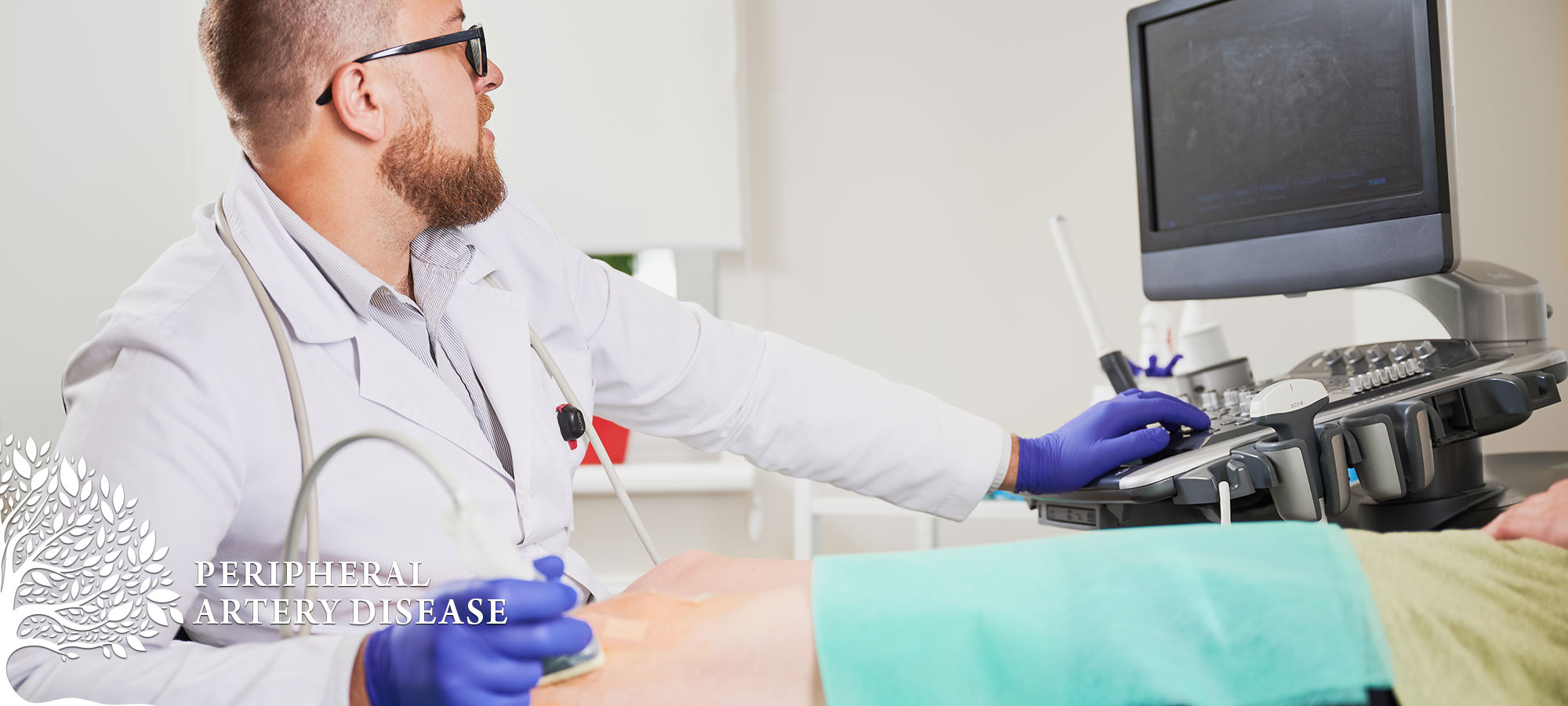
Peripheral Artery Disease
A cardiovascular condition known as peripheral arterial disease (PAD) occurs when plaque build up increases within the arteries , lowering blood flow to the limbs. PAD is a dangerous illness that frequently remains untreated until symptoms appear.
Causes of Peripheral Artery Disease
Peripheral artery disease (PAD) occurs when fatty deposits accumulate on the artery walls, limiting blood flow. This condition, called atherosclerosis, affects the arteries that supply blood to the limbs. Key risk factors include smoking, diabetes, obesity, high blood pressure, and a family history of heart disease.
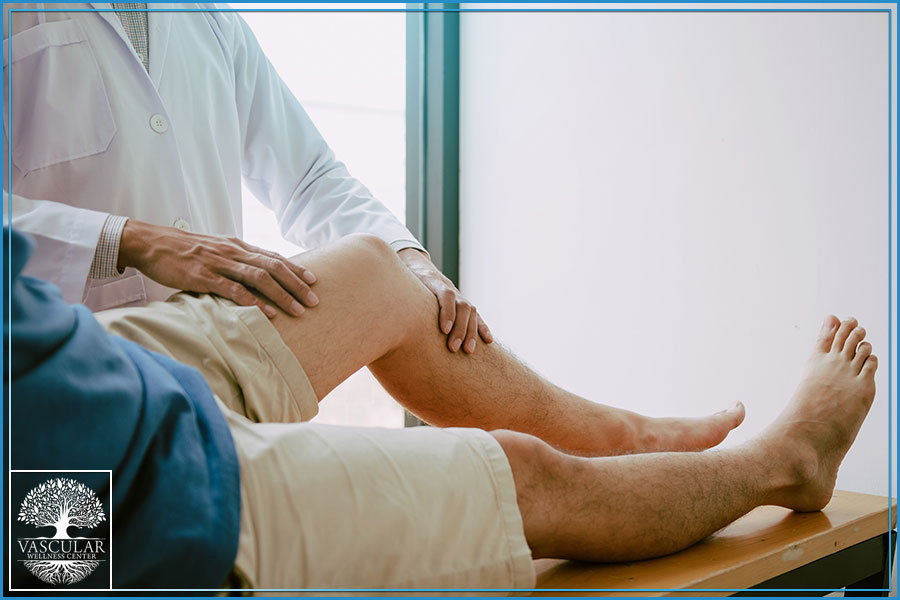
Peripheral Artery Disease Symptoms & Risk Factors
Early diagnosis, the development of a treatment plan, and prompt intervention in the event of severe symptoms all depend on the ability to recognize the signs and symptoms of peripheral arterial disease. Pain while walking is a common presenting symptom for many people. Nevertheless, 40% of people with PAD arrive with no symptoms or attribute their leg problems to causes other than PAD. You should get assessed if you get excruciating leg cramps that go away when you rest and come back when you walk. Patients with peripheral arterial disease (PAD) can have a satisfactory outcome with an active treatment strategy and an early diagnosis.
Common Signs and Symptoms for Peripheral Artery Disease include:
- Leg muscle fatigue, heaviness, or cramping
- Pale, discolored, or bluish toes or feet
- Leg or foot pain interrupting sleep
- Sores on toes, feet, or legs that heal slowly or not at all
- One leg or foot colder than the other
- Thickened, yellow toenails with slow growth
Do you have risk factors for Peripheral Artery Disease?
- Smoking
- Diabetes
- Kidney Disease
- High Blood Pressure
- High Cholesterol
- Advanced Age
If you or a loved one has leg pain, numbness, non-healing sores, or weakness, seek medical evaluation promptly.
Peripheral Artery Disease Diagnosis:
Diagnosis involves a medical history review, physical exam, and an ankle-brachial index (ABI) test, which compares blood pressure in the legs and arms. A significant difference can indicate PAD.
Additional Diagnostic Tests For PAD:
- Ultrasonography
- Magnetic Resonance Angiography (MRA)
- Computed Tomographic Angiography (CTA)
- Peripheral Diagnostic Angiogram
Severe PAD Complications:
Advanced PAD can cause significant tissue damage due to poor blood flow, leading to open sores, gangrene, and critical limb ischemia (CLI), which raises the risk of limb loss and life-threatening events like heart attacks or strokes.
How to Take Action to a Peripheral Artery Disease Diagnosis:
Initial treatment involves lifestyle changes and medications. If these do not improve the condition, surgical interventions such as angioplasty or stent placement may be recommended. Early diagnosis and an active treatment plan can prevent severe complications, including amputation.
PAD Treatment Options:
- Lifestyle changes (quitting smoking, exercising, healthy diet)
- Medications (cholesterol control, blood pressure management, blood sugar control)
- Endovascular or surgical procedures (angioplasty, stent placements, atherectomies)

Preventing PAD:
Preventative strategies include regular exercise, a diet low in saturated fats, maintaining a healthy weight, quitting smoking, and controlling blood sugar for diabetics.
PAD Progression:
Without treatment, PAD can lead to critical limb ischemia (CLI) and increase the risk of limb amputation.
FAQs About PAD:
Can PAD affect life expectancy?
Yes, without treatment, PAD can shorten lifespan, but it can be managed with lifestyle changes, medications, and interventions.
What does PAD feel like in the legs?
Pain, numbness, dry skin, and non-healing wounds are common symptoms.
How does PAD affect the toes?
Pain, numbness, dry skin, slow-growing nails, and gangrene can occur due to poor circulation.
Why does PAD cause skin discoloration?
Reduced oxygen flow can cause vessel damage, scarring, and darkened skin.
Can arterial plaque be reversed?
Lifestyle changes and risk management can help control and reduce plaque buildup.
What causes plaque buildup?
Fat deposits and inflammation in artery walls can lead to scarring and calcium buildup, hardening the arteries.
